This is my free weekly newsletter covering 5 interesting points from the week. Subscribe (if you haven’t already) if you’d like to get it in your inbox each week!
1. Optimism is associated with “exceptional” longevity
August 2019 study: Optimism is associated with exceptional longevity in 2 epidemiologic cohorts of men and women
Previous studies reported that more optimistic individuals are less likely to suffer from chronic diseases and die prematurely.
…In conclusion, we found higher optimism levels were associated with longer life span and greater likelihood of achieving exceptional longevity.
Data on Women from the Nurses’ Health Study (2004 to 2014) and men from the Veterans Affairs Normative Aging Study(1986 to 2016) found that optimism is related to 11 to 15% longer lifespan on average. “Participants with highest versus lowest optimism levels had 1.5 (women) and 1.7 (men) greater odds of surviving to age 85.”
2. Eating late increases your risk for anxiety and depression?
July 2024 study: Dietary Rhythmicity and Mental Health Among Airline Personnel
This cross-sectional study found that meal timing, long eating window, and meal jet lags were associated with increased odds of depression and anxiety.
Data on Chinese pilots, flight attendants and air security officers (aged 18 to 60) reveals that having dinner after 8pm on morning-shift, night-shift or rest days was associated with a higher risk of anxiety and depression compared with eating before 8pm. An eating window of less than 12 hours was associated with reduced risk of anxiety and depression on morning-shift and rest days.
3. The body needs MORE Protein when repairing
July 2024 study: Association between protein intake and functional capacity in critically ill patients: A retrospective cohort study
A study on patients in the ICU for more than 7 days between October 2014 and September 2020 found that a dose of protein 1.2-1.5g/kg/day was associated with superior functional capacity at discharge compared with lower doses. The RDA is much lower than this - 0.8g/kg/day.
They also noted that this was not just a matter of undernourished people finally getting enough nourishment: “The high group had superior CPAx in both well-nourished and malnourished patients, indicating nutrition status was not an effect modifier.”
4. Messing up your circadian rhythm messes up your back?
January 2020 paper: The circadian rhythm in intervertebral disc degeneration: an autophagy connection
It’s very common for me to stay up very late, sometimes through to the next morning when I am putting the final touches on a video right before uploading. More than once, I’ve noticed some unexpected back pain that would usually resolve when I slept properly. I was always curious about the mechanism, and this paper might be a clue to that.
Disruption of molecular activities that follow a 24-hour cycle, known as a circadian rhythm, can promote the degeneration of the discs between vertebrae by affecting the natural degradation of cellular components known as autophagy.
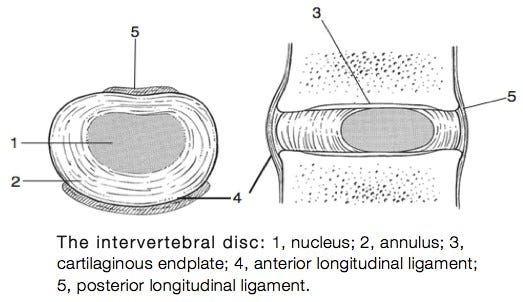
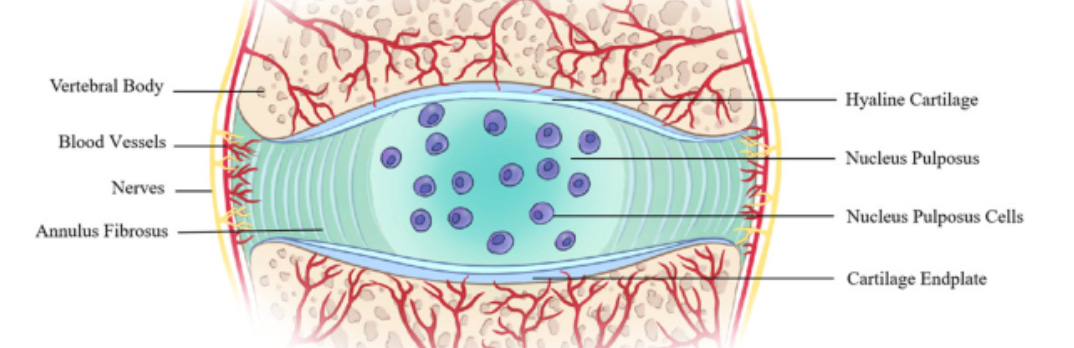
About 2/3rds of adults suffer from lower back pain with the most common reason for this being age-related degenerative processes in the intervertebral discs as well as intervertebral disc herniations. This paper out of Experimental and Molecular Medicine explains that a molecular clock has been found in intervertebral discs and that when this clock is disrupted it can stress the nucleus pulposus cells (see purple blobs below) in the disc which then contributes to the degeneration of these intervertebral discs. They explain that autophagy occurs in these nucleus pulposus cells and that autophagy is strongly affected by the circadian rhythm. That is, disc degeneration may be exacerbated by the process of autophagy being perturbed by an unhealthy circadian rhythm.
Night shift work also involves abnormal loading/resting cycles. In these cycles, intervertebral discs undergo changes in the mechanical loading and activation of autophagy, which can result in intervertebral disc degeneration.
5. Vitamin K2 protects your teeth and gums
November 2023 study: A Case Control Study Evaluating the Relationship between Vitamin K2 Serum Level and Periodontitis
Vitamin K2 (VK2) is an essential co-factor for bone metabolism. There is still very little data regarding possible VK2 relation to periodontitis.
I’ve talked in previous videos about how fat soluble vitamins are very important for skeletal development. Here we have a paper investigating the link between levels of the fat soluble vitamin Vitamin K2 and gum disease (periodontitis) progression. They compared 50 patients with periodontitis to 50 people without it.
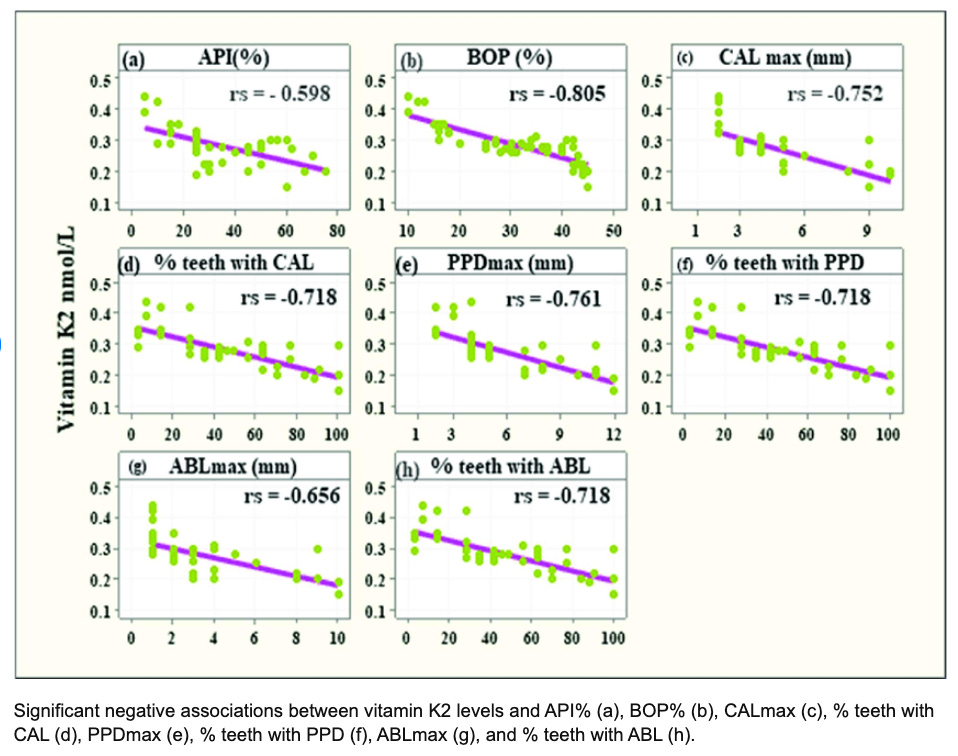
Patients with periodontitis had mean serum levels of VK2 significantly lower (0.27 ± 0.06 nmol/L; p < 0.001) than the control group (0.43 ± 0.09 nmol/L; p < 0.001) regardless of the patient’s age or sex. The VK2 serum level decreased with the severity of periodontitis with the lowest level in stage IV of the disease (0.19 ± 0.01 nmol/L; p < 0.001).
Simply put: The lower their vitamin K2 levels, the worse their gum disease.
In the present study, the VK2 serum level was correlated to periodontitis, and its severity, complexity, extension, and grade. The range of VK2 was decreasing together with the worsening of all clinical parameters of periodontitis.








I keep seeing more benefits regard K2 as time goes on, which is neat as it's a supplement I am taking since a while ago. It's very/quite cheap like Creatine, so might as well.
Thanks so much Joseph once again. 'Love the piece on protein. As the mantra goes, "protein is for structure, fat is for energy". Immobilization, such as in a hospital, is a real killer. Patients lose muscle mass at a rapid rate just from immobilization, and former ICU patients can end up with long lasting physical and and also Mental disability (called Post-Intensive Care Sydrome/ PICS). Vanderbilt's Dr. E.W. Ely has been a pioneer in preventing harm from ICU care, in particular ICU-aquired brain disease. He has campaigned for protocols to encourage movement in ICU patients (for instance, even intubated patients can walk through their hospital ward with enough assistance). Increasing protein in the tube feedings (TPN) may help lower the need for such labor-intensive movement protocols though! TPN is notoriously nutrient-deficient, and patients can develop beriberi and other deficiencies when depending on it. TPN uses poor quality oils as well, instead of omega-3 oil for example. Moral of the story: stay out of the hospital!