This is my free weekly newsletter covering 5 interesting points from the week. Subscribe (if you haven’t already) if you’d like to get it in your inbox each week!
1. Vegetable fat is bad for lemur brains
A May 2024 study found that when pregnant lemurs are fed a vegetable fat-based diet cognitive development in their children is impaired, compared to the mothers receiving a dairy-fat based diet.
Across all tasks, we observe more successful neonates born to mothers fed a DF diet. A greater rate of falls is observed in 8-day-old VF neonates, which is associated with delayed psychomotor development. Our findings suggest the potential benefits of lipids originating from a lactovegetarian diet compared with those originating from a vegan diet for the psychomotor development of neonates.
The authors point to the inferiority of a vegan diet.
2. The ketogenic diet heals the brain
The debate on whether the ketogenic diet is better for weight loss than just calorie cutting has taken attention away from the more impressive aspects of the diet. Namely, it is very good for the brain because it is very good for mitochondria.
A good illustration of the substantial beneficial effect the diet has on the mitochondria is Parkinson’s disease.
Mitochondrial dysfunction has long been suspected to be key to the development of Parkinson’s disease. This is illustrated clearly by survivors of cyanide poisoning. Cyanide rapidly kills people by simply interfering with a step in the energy production process in the mitochondria. Not many people survive a cyanide poisoning, but there are case reports discussing cyanide induced parkinsonism. After the cyanide rips through their mitochondria, some survivors are left with Parkinson’s.
The ketogenic diet is beneficial for mitochondria is that it has neuroprotective effects in the case of Parkinson’s. The diet reduces muscle stiffness and improves cognitive function.
In Chapter 11 of the textbook Nutrition and Traumatic Brain Injury, they note that:
“…the ketogenic diet has been further shown to be neuroprotective in animal models of several central nervous system (CNS) disorders, including Alzheimer’s disease (AD), Parkinson’s disease, hypoxia, glutamate toxicity, ischemia, and traumatic brain injury (TBI) (see Prins, 2008, for a review)…”
They explain that the ketogenic diet is beneficial for the brain through various mechanisms:
-Stimulates the production of new mitochondria
-Provides alternative fuels for the brain
-Increases GABA
-Reduces the production of reactive oxygen species (Basically the mitochondrial engines are burning fuel more cleanly)
The benefits to the mitochondria are hard to put in perspective, so let’s take a look at ALS, or Lou Gherig’s Disease. ALS (the disease that Stephen Hawking had) is where motor neurons die, leading to dramatic weakening of the muscles. It’s thought that in ALS, motor neurons die via mitochondrial dysfunction. So could ketosis’s mitochondrial benefits help in this case?
Well, in a rat model of ALS, the ketogenic diet slowed the progression of ALS by half.
KD fed mice lost 50% of baseline motor performance 25 days later than disease controls. KD animals weighed 4.6 g more than disease control animals at study endpoint; the interaction between diet and change in weight was significant (p = 0.047). In spinal cord sections obtained at the study endpoint, there were more motor neurons in KD fed animals (p = 0.030).
The research on keto for ALS is in its early stages, but a case report on one (human) man with ALS reveals that a time-restricted ketogenic diet normalized his depression and stress levels, improved his ALS-related function by 7%, his forced expiratory volume by 17% and improved his fatigue by 23%. “His swallowing impairment and neurocognitive status remained stable.” The authors conclude that “Now over 45 months since symptom onset, our patient remains functionally independent and dedicated to his TRKD.”
3. Plant-based diet is better for the gut? Not so fast.
“Alpha diversity” in the context of gut health means that there is a wide variety of microbial species comprising the gut microbiome. This is generally associated with health benefits thanks to a more resilient and stable gut microbiome.
What is said to be the best thing for the gut microbiome? Plants, of course.
In a 2014 study, 10 healthy human volunteers were placed on a short-term plant-based diet (PBD) consisting of 300 g of carbohydrate per day from cereal, vegetables, rice, lentils, and fruit or on an animal-based diet (ABD) consisting of less than 3 g of carbohydrates per day, with 30% of calories from protein and 70% of calories from fat from eggs, meat, and cheese. While distinct gut microbial communities emerged in both groups, there was no significant change in alpha-diversity in either group.
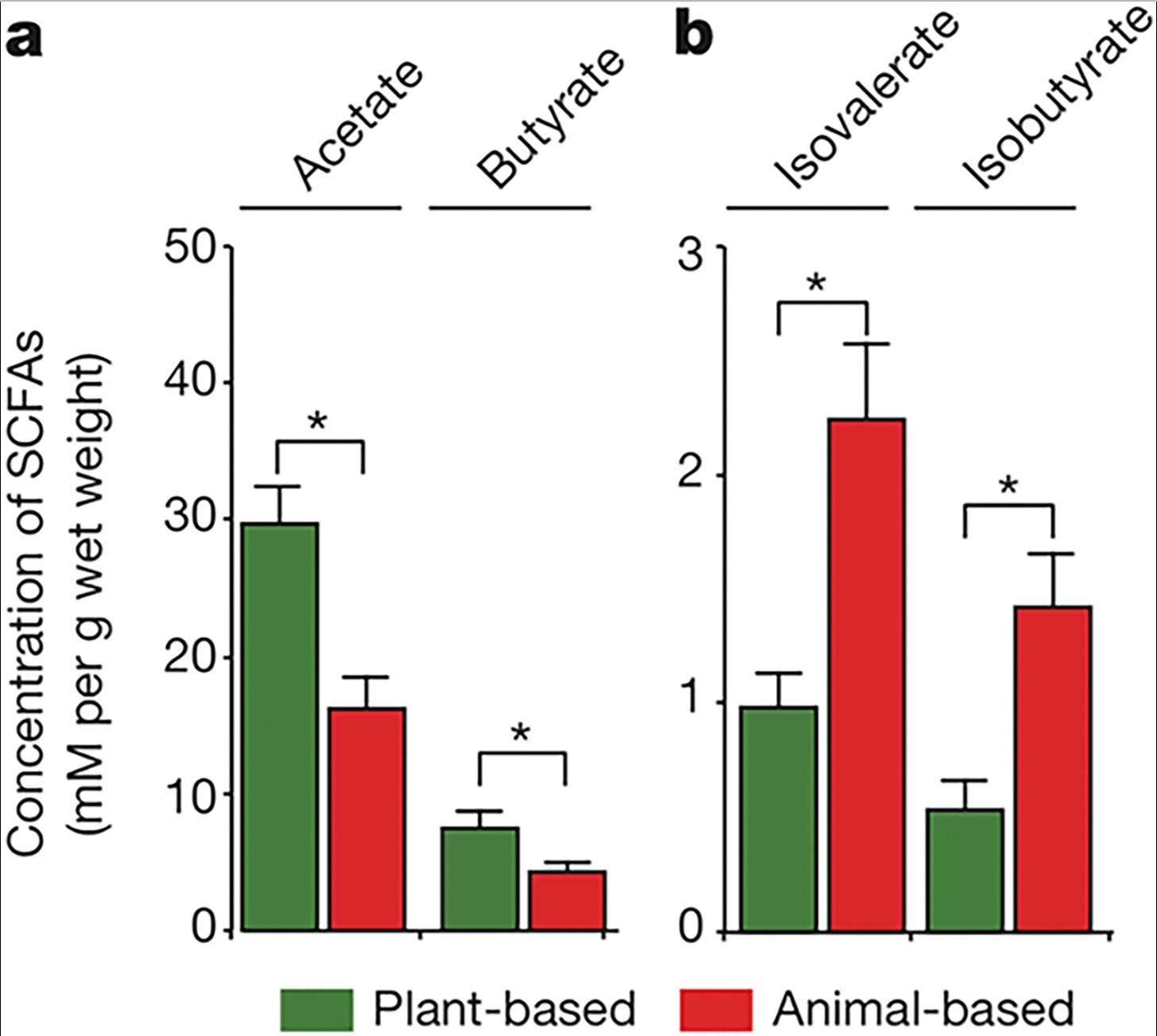
One argument in favor of plant-based diets being good for the gut is increased production of butyrate from the microbes metabolizing plant carbohydrates. However, in this study, the plant-based diet group only produced a bit more butyrate than the animal based group, but the animal-based group produced substantially more isovalerate and isobutyrate.
Considering isobutyrate has been shown to activate many of the same receptors as butyrate, the animal-based diet arguably achieved a better result for the gut. Also note that the subjects in the animal-based diet group were were confirmed to be in ketosis by day 2 of the diet, which would give them plenty of betahydroxybutyrate.
4. PTSD wasn’t a thing for Hunter Gatherers?
In the textbook Evolutionary Psychology, the authors explain that a particular hunter gatherer population isn’t as susceptible to PTSD despite being exposed to similarly tragic events.
They argue that part of the physiological changes that come along with PTSD are increased inflammation in the body. Thus, the inflammatory nature of a standard western diet may exacerbate PTSD:
It seems that contemporary Western lifestyles and low-grade inflammation change previously adaptive PTSD into a non-adaptive state of MDD by incorporating symptoms of sickness behaviour with PTSD, probably aggravating PTSD symptoms (Rantala et al., 2018).
A 2020 study on Turkana warriors in Kenya found them to be much less likely to develop PTSD-related symptoms compared to US combat vets despite also experiencing gruesome acts in a war zone.
In contrast to people with contemporary Western lifestyles, Turkana warriors have excellent cardiometabolic health (Lea et al., 2020), suggesting that they do not suffer from low-grade inflammation.
They note that certain lifestyle factors as well as nutrition affect the risk of chronic PTSD.
…smoking, obesity and low physical activity increase the risk of chronic PTSD (Buckley et al., 2004; Olff et al., 2006), while micronutrient intake may decrease it (Rucklidge et al., 2012). Thus, although PTSD per se seems to be an adaptation caused by natural selection to avoid the cause of the trauma, it seems that the depression triggered by PTSD is a pathological consequence caused by modern Western lifestyles (Rantala et al., 2018).
5. Carnitine and depression
A 2014 review of four randomized trials found that supplemental carnitine shows promise for treating depression. Considering that placebos can confer measurable benefits to depression and that there was only a “small” difference in the effectiveness of antidepressants over placebo, it’s impressive that carnitine performed better than placebo.
“Endogenous L-carnitine (LC) and its derivative acetyl-L-carnitine (ALC) play antidepressant roles by improving brain energy metabolism, regulating neurotransmitters and neural plasticity.” (S)